At Microsoft’s AI for Good Lab, we’ve been working with companions on the College of Washington, the Fred Hutchinson Most cancers Heart, and different establishments to discover whether or not synthetic intelligence may also help convey better readability, accuracy, and belief to breast most cancers screening.
This week, our joint analysis workforce launched the outcomes of a brand new research revealed in Radiology, detailing a promising AI method that goals not simply to detect most cancers—however to take action in a means that radiologists can belief and sufferers can perceive.
The challenges with current breast cancer screening
Breast most cancers is the commonest most cancers amongst girls worldwide. In the USA alone, one in eight girls shall be recognized with breast most cancers in her lifetime. Early detection via screening is essentially the most highly effective device obtainable to save lots of lives, with a 20% to 40% discount in mortality for girls aged 50-69—but it stays an imperfect science.
Magnetic Resonance Imaging (MRI) is among the many most delicate screening instruments obtainable, particularly for girls at increased danger. However for all its sensitivity, MRI comes with severe trade-offs: excessive charges of false positives, considerably elevated anxiousness for sufferers, and pointless biopsies. The issue is particularly acute for the practically 50% of girls who’ve dense breast tissue—a situation that not solely will increase the danger of breast most cancers but additionally makes it more durable to detect abnormalities via conventional imaging strategies like mammograms.
Too typically, these challenges translate right into a troubling equation: extra scans, extra uncertainty, and extra follow-up procedures that change into pointless. In reality, solely a small fraction—lower than 5%—of girls present process breast MRI screening are finally recognized with most cancers.
A smarter model, built for the real world
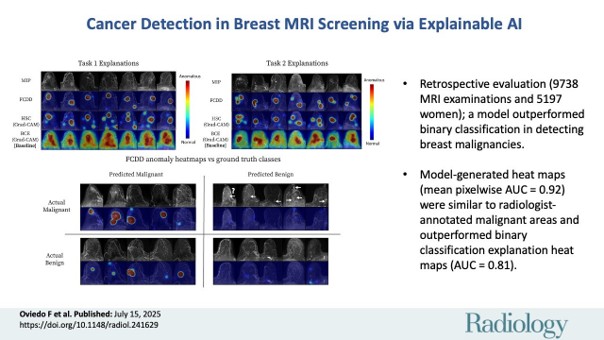
The mannequin—known as FCDD (Totally Convolutional Information Description)—is predicated on anomaly detection fairly than customary classification. That’s an essential shift. As a substitute of attempting to study what each potential most cancers appears to be like like, the mannequin learns what regular breast scans appear to be and flags something that deviates.
This method is especially efficient in real-world screening settings the place most cancers is uncommon and abnormalities are extremely assorted. Throughout a dataset of over 9,700 breast MRI exams, the mannequin was examined in each high- and low-prevalence situations—together with practical screening populations the place simply 1.85% of scans contained most cancers.
Right here’s what we discovered:
- Improved accuracy in low-prevalence populations: FCDD outperformed conventional AI fashions in figuring out malignancies whereas dramatically lowering false positives. In screening-like settings, it achieved double the optimistic predictive worth of ordinary fashions and minimize false alarms by greater than 25%.
- Distinctive explainability: In contrast to most AI fashions, FCDD doesn’t simply give a “sure” or “no”—it generates heatmaps that visually spotlight the suspected tumor location within the two-dimensional MRI projection. These rationalization maps matched professional radiologist retrospective annotations with 92% accuracy (pixel-wise AUC), far exceeding different fashions.
- Generalizability throughout establishments: With out retraining, the mannequin maintained excessive efficiency on a publicly obtainable exterior dataset and an impartial inside dataset, suggesting robust potential for broader medical adoption.
Making AI impactful, not just impressive
This mannequin is greater than a technical achievement. It’s a step towards making AI helpful in medical workflows—offering triage help, lowering time spent on regular circumstances, and focusing radiologists’ consideration the place it issues most. By enhancing specificity at excessive sensitivity thresholds (95–97%), the mannequin may assist scale back pointless callbacks and biopsies, easing emotional and monetary burdens for sufferers.
Importantly, the code and methodology have been made open to the analysis neighborhood. You possibly can discover the venture right here: GitHub Repository, and the paper right here.
As with all AI in healthcare, the trail to impression requires greater than algorithms. It requires belief. Belief is constructed not solely by efficiency metrics but additionally by transparency, interpretability, and a transparent understanding of the medical context wherein these instruments are deployed.
The place we go from here
We nonetheless have work forward. The mannequin will have to be examined prospectively in bigger, various medical populations. However the outcomes are promising—they usually mark an essential shift in how we take into consideration the position of AI in drugs. Relatively than asking medical doctors to belief a black field, we’re constructing fashions that shine a lightweight on what they see and why.
“We’re very optimistic concerning the potential of this new AI mannequin, not just for its elevated accuracy over different fashions in figuring out cancerous areas however its skill to take action utilizing solely minimal picture knowledge from every examination. Importantly, this AI device will be utilized to abbreviated contrast-enhanced breast MRI exams in addition to full diagnostic protocols, which can additionally assist in shortening each scan instances and interpretation instances,” mentioned Savannah Partridge, Professor of Radiology on the College of Washington and senior creator of the research. “We’re excited to take the subsequent steps to evaluate its utility for enhancing radiologist efficiency and medical workflows.”
AI is not going to change radiologists. However with the fitting design and oversight, it may give them sharper instruments and clearer alerts to extend confidence in evaluating tough circumstances.
Breast most cancers is a worldwide problem. With AI, we’ve got an opportunity to detect it earlier, scale back pointless interventions, and finally save extra lives. That could be a future value constructing towards—one pixel, one scan, and one breakthrough at a time.